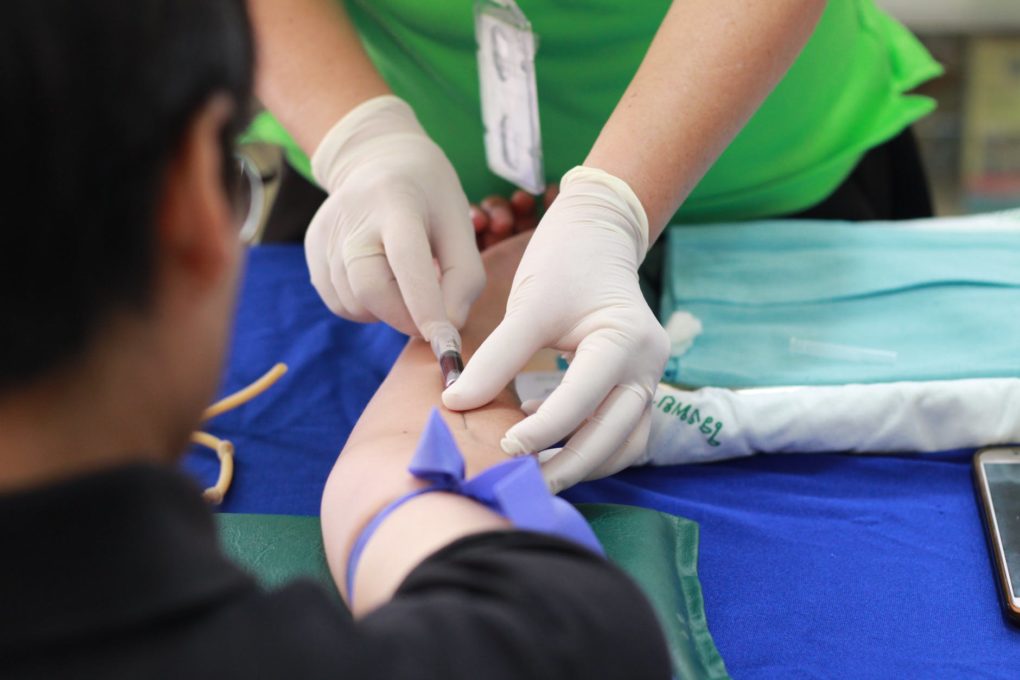
CNA Shortage Fuels Rise In Patient Mistreatment
CNAs play a critical role in our healthcare system, assisting licensed nurses, aiding patients with their activities of daily living, and even providing home healthcare support and housekeeping assistance in assisted living facilities and nursing homes. Simply put, CNAs keep our healthcare systems running. Unfortunately, there aren’t nearly enough CNAs to meet demand and the lack of qualified professionals is putting patients at risk.
Without enough CNAs, patients often go without necessary care, especially in nursing homes where the majority of daily support is provided by CNAs. Some nursing homes even resort to sedating patients with antipsychotics to reduce demands and save time – while other facilities devolve to the point that patients are badly neglected, suffering serious infections, or are even subject to abuse by undertrained, overworked staff.
If our medical system is going to resolve its CNA shortage, it’s going to take a multipronged approach, including better education and changes to staffing standards, and some facilities are already working hard to retain their best staff. Particularly faced with an aging population, CNAs are in high demand. Meeting that call will be one of the greatest challenges over the next several years.
Training New CNAs
While improving conditions for current CNAs, the first thing our healthcare system needs to do if it’s going to meet demand for these core staffers is to train more new CNAs. Luckily, CNA training programs are widely available and generally affordable, and once they’re completed, CNAs can find jobs in hospitals, with home health agencies, and in various residential facilities. There are many excellent opportunities, and this is part of what makes it so difficult for residential facilities to retain the best CNAs; hospitals usually pay more and are better staffed.
Incentivizing Retention
Faced with a shortage of CNAs compared to demand, care facilities have developed a variety of strategies to reduce turnover, and the most successful programs start with the hiring process. For example, many CNAs think that nursing homes are relatively low stress – until they start working at one and discover that they’re dealing with very sick, demanding patients. It’s important for hiring managers to carefully observe CNA applicants during their visits to see how they respond to the facility and listen carefully to how they talk about the residents. Facilities that can successfully find people who are passionate about nursing home-based care are more likely to maintain adequate staffing levels and to have a satisfied team.
In addition to making changes at the facility level, some states are addressing staffing challenges by modifying their licensing process. This year, New Jersey changed its laws to allow CNAs to practice with out-of-state licenses. This type of reciprocity law acknowledges both the overall shortage of CNAs and other types of nurses and the general similarity of CNA training programs across the country. Barring a professional from practicing in a high-demand, understaffed field because they studied in a different state is simply untenable in a crisis like this.
The US population is rapidly aging, with 10,000 baby boomers turning 65 every day, and not only is our population aging, but we’re also living longer. Unfortunately, living longer and living better are not the same thing, and that means more older adults are living for years with serious health conditions. CNAs may need more advanced training to properly support these patients, and both Medicaid and facilities will need more funding to support increased demand.
The CNA industry is in need of reform across the board, and there’s little time for the field to adapt. For now, facility-by-facility change may be the best we can hope for, and those who change their norms successfully are most likely to thrive as the industry takes on its new shape.
Subscribe for natural health news to your inbox. Follow Natural Blaze on YouTube, Twitter and Facebook.